Menopos at Mga Pagbabago sa Hitsura ng Peklat
Understanding the physiological shift behind Menopos at Mga Pagbabago sa Hitsura ng Peklat requires looking past the surface-level frustration at the complex, often invisible breakdown of the skin’s structural integrity.
patalastas
When estrogen levels plummet, the body doesn’t just stop producing moisture; it fundamentally rewrites the blueprint of how our dermal layers hold together, turning once-faint memories of old injuries into vivid, textured reminders.

Table of Contents
- The Estrogen Deficit: Why Old Scars Re-emerge
- Collagen Depletion and the Architecture of the Dermis
- Comparative Recovery: The Shift in Healing Velocity
- Clinical Strategies for Mature Skin Restoration
- Common Inquiries Regarding Hormonal Skin Shifts
Why Does Estrogen Loss Redefine Your Skin’s History?
Hormonal fluctuations during the perimenopausal transition do more than just trigger hot flashes; they initiate a systemic overhaul of cutaneous physiology.
Estrogen is the primary architect of skin hydration and elasticity. Its sudden absence leaves the skin thinner and more translucent, which effectively “shines a light” on underlying fibrous tissue that was previously masked by a plump, youthful dermis.
Existing scars often become more prominent because the surrounding tissue loses the volume that once kept the skin’s surface level. It is a common misconception that scars are static.
patalastas
In reality, Menopos at Mga Pagbabago sa Hitsura ng Peklat are driven by a sharp decline in mucopolysaccharides.
Without these molecules to retain water, the skin becomes brittle, making old keloids or surgical lines appear sharper and more pronounced against a drying landscape.
Beyond the visual shift, there is a sensory one. Lowered estrogen concentrations drag down the rate of re-epithelialization—the skin’s natural resurfacing mechanism.
Women often report that scars which remained dormant for decades suddenly feel “active” again, becoming darker, redder, or developing a persistent, nagging itch.
This isn’t just vanity; it’s an inflammatory response. The hormonal shift creates a more reactive environment within the skin’s layers, prolonging the vascular phase of healing.
Clinical observations frequently show that the blood vessels within old scar tissue can become more dilated, leading to a lingering redness that makes an old mark look surprisingly recent.
Collagen Degradation: The Collapse of Structural Support
Collagen is the scaffolding of the human frame, yet the first five years of the menopausal transition see a staggering 30% loss of this essential protein.
This collapse is the primary engine behind Menopos at Mga Pagbabago sa Hitsura ng Peklat. When the support beams of the skin fail, the surface begins to sag and fold, often creating deep troughs around existing scars.
Atrophic scars—those slight indentations from past acne or chickenpox—frequently deepen during this period.
As the subcutaneous fat pads diminish, the natural “cushion” that kept these scars flush with the skin disappears.
++ Paano Binabago ng Menopos ang Thermosensitivity sa Sikat ng Araw
Conversely, hypertrophic scars may feel more restrictive; without adequate moisture, the collagen fibers within the scar tissue become rigid rather than resilient.
While the market is flooded with peptide creams, topical fixes rarely compensate for a systemic hormonal crash.
Advanced dermatological data suggests that without estrogen’s regulatory influence, new collagen fibers are laid down in a disorganized, chaotic fashion.
This lack of architectural oversight results in a skin texture that feels uneven and highlights every previous imperfection.
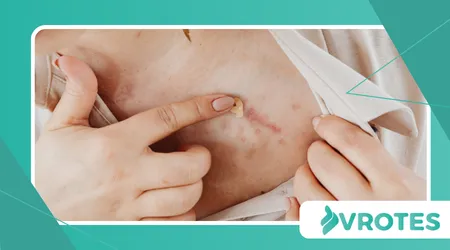
The Evolution of Healing Capacity
Navigating Menopos at Mga Pagbabago sa Hitsura ng Peklat requires a mental shift in how we perceive recovery. The body’s regenerative timeline is no longer what it was in your thirties.
Healing markers, such as TGF-beta, fluctuate in ways that favor the production of tough fibrous tissue over smooth, integrated skin cells.
Recent 2026 data indicates that cellular turnover slows dramatically, extending the “remodeling phase” of a scar from a few months to several years.
Read more: Mga Pagbabago sa Komposisyon ng Pawis Pagkatapos ng Menopause
The following data highlights the physiological shifts that occur during this transition and their specific impact on the skin’s surface.
Healing Dynamics: Pre-Menopause vs. Post-Menopause
| Physiological Factor | Premenopausal Baseline | Postmenopausal Shift (2026 Data) | Visual Impact on Scars |
| Collagen Content | High/Stable | 2.1% annual decline | Increased depth and wrinkling |
| Skin Thickness | Robust Dermis | ~1.1% thinning per year | Scars appear more “raised” |
| Hydration (GAGs) | High Retention | Significant Moisture Loss | Scars become itchy/flaky |
| Healing Velocity | Rapid Recovery | 25-40% slower turnover | Prolonged redness/pigment |
Refining the Appearance of Mature Scar Tissue: Menopause and Scar Appearance Changes
Managing Menopos at Mga Pagbabago sa Hitsura ng Peklat effectively involves a transition from basic skincare to clinical-grade intervention.
++ Paano Pinapabuti ng Paglalakad ng Hapon ang Lakas sa Menopos
Silicone sheeting remains a primary recommendation for flattening raised tissue because it creates a synthetic “micro-climate” that traps moisture, mimicking what the body used to do naturally.
Energy-based treatments like fractional lasers or microneedling can be used to “reset” the area. By creating controlled micro-injuries, these tools force the skin to produce organized collagen fibers to replace the old, brittle ones.
However, these procedures require a skilled hand, as mature skin is more prone to bruising and requires longer downtime.
Hydration remains the most underestimated variable. Well-hydrated skin reflects light more evenly, blurring the harsh edges of surgical marks or old injuries.
Prioritizing ceramides and hyaluronic acid helps fortify the skin barrier against environmental stressors that typically make scars look worse.
According to the American Academy of Dermatology, UV protection is the single most important factor in scar maintenance.
Sun exposure induces permanent hyperpigmentation in compromised tissue, causing scars to turn a dark, muddy brown that contrasts sharply with the thinning skin typical of the menopausal years.

FAQ
Why has an old scar suddenly started itching?
The drop in estrogen levels results in a compromised lipid barrier and extreme dryness. This lack of oil production causes old scar tissue—which lacks sweat glands and hair follicles to begin with—to become tight and irritated. High-quality emollients are usually enough to soothe this neurological sensitivity.
Is there a higher risk of keloids during this stage?
While keloids are primarily a genetic predisposition, the prolonged inflammation associated with Menopos at Mga Pagbabago sa Hitsura ng Peklat can lead to hypertrophic scarring.
Surgeons often advocate for proactive postoperative care, such as early silicone application, for patients in this demographic to prevent excessive scar build-up.
Does Hormone Replacement Therapy (HRT) improve scars?
HRT can significantly improve skin thickness and moisture retention, which makes the skin more resilient and masks the depth of scars. While not a primary reason to seek hormone therapy, the improvement in skin quality is a documented secondary benefit for many women.
Reframing the Narrative
The reality is that Menopos at Mga Pagbabago sa Hitsura ng Peklat are an inevitable byproduct of a shifting endocrine system. But visibility doesn’t have to mean vulnerability.
By acknowledging that the skin is now in a more delicate, transparent phase, you can pivot your routine toward protection and structural support.
Technology in 2026 offers more sophisticated ways to manage these transitions than ever before. Whether through bio-identical topicals or regenerative clinical procedures, you have the agency to ensure your scars remain a subtle part of your story rather than its focal point.
Always consult a specialist when introducing clinical-grade treatments to ensure they align with your specific hormonal profile.
For those interested in the deeper biological mechanisms of skin aging, the National Institutes of Health provides extensive archives on cutaneous hormonal research.
++ Why Do Scars Flare Up During Menopause?
++ Beyond Hot Flashes: Understanding and Treating Menopause-Associated Skin Changes
